US employers expect to see biggest jump in healthcare costs in a decade next year
Three healthcare benefit consulting firms are forecasting costs to rise 5.4% to 8.5% in 2024
Americans want self-determination when it comes to health choices: Rep. Richard McCormick
Rep. Richard McCormick, R-Ga., a member of the GOP doctors caucus, discusses White House COVID protocols and questions surrounding Sen. Mitch McConnell's health.
Employers in the U.S. are expecting to see the largest increase in healthcare costs in a decade in 2024, according to forecasts from healthcare benefit consultants — although workers may avoid some of the increase due to the tight labor market.
Benefit consultants from Mercer, Aon and Willis Towers Watson see employers’ healthcare costs jumping by a range of 5.4% to 8.5% in 2024 because of medical inflation, high demand for expensive weight-loss drugs and the wider availability of high-priced gene therapies.
Over two-thirds of employers either don’t plan to shift any cost increases to their staff or will pass on less than the expected cost increase in 2024, according to a survey by Mercer, a unit of Marsh McLennan.
BIDEN ADMIN NAMES FIRST 10 DRUGS SUBJECT TO MEDICARE PRICE NEGOTIATION

Dr. Jay Itzkowitz, head of the emergency department, and Margaret Puya, RN, are seen in the new Trauma Unit at Mount Sinai South Nassau hospital in Oceanside, New York, on Jan. 26, 2023. (Hoard Schnapp/Newsday RM via Getty Images / Getty Images)
"They don’t want to add more financial stress on employees who are also coping with inflation, especially in this time where they’re really relying on their health benefits as a way to keep employees working for them," said Beth Umland, Mercer’s director of health and benefits research.
The U.S. economy has been confronted with high consumer prices over the last year amid inflation stemming from pandemic-era spending levels and supply chain shortages. Inflation ticked up to 3.7% over the past 12 months through August, down from a 40-year high of 9.1% in June 2022.
But cost increases in the healthcare sector tend to lag economy-wide inflation due to contracts between insurers and providers such as hospitals that cover the prices for various procedures and are signed months or years in advance.
DIABETES DRUG TESTED FOR WEIGHT LOSS COULD BE GAME CHANGER
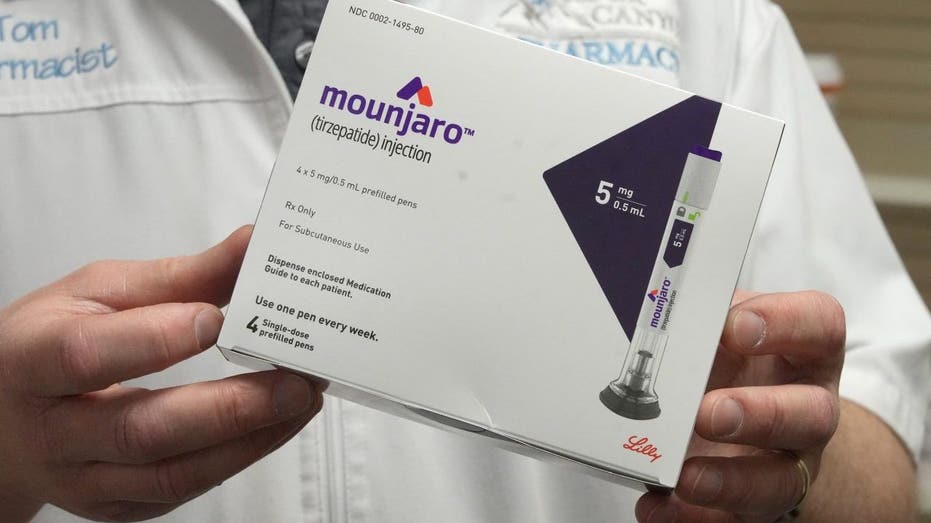
Demand has surged for Mounjaro and other diabetes drugs as weight loss treatments over the past year, contributing to the projected rise in healthcare expenses. (REUTERS/George Frey / Reuters Photos)
Benefit consultants help medium and large employers design their healthcare coverage plans for employees. Roughly two-thirds of U.S. workers get their benefits from such plans.
Aon projected an 8.5% increase in employer healthcare costs next year, with 1 percentage point of the total coming from weight-loss drugs alone. Sales of Novo Nordisk’s Wegovy, which is approved to treat obesity, as well as "off-label" use of similar diabetes drugs like Novo’s Ozempic and Eli Lilly’s Mounjaro for weight loss have surged amid high demand over the last year.
About half a dozen gene therapies have been approved for use by U.S. regulators over the last year, most of which cost over $1 million — which the consultants noted could significantly raise costs for a company if just one employee undergoes gene therapy treatment.
GET FOX BUSINESS ON THE GO BY CLICKING HERE
All the consultants noted that employers will increasingly use artificial intelligence (AI) to reduce administrative staff expenses and added that there will be greater scrutiny of coverage for expensive therapies.
Businesses and insurers are also working to identify less expensive hospital networks for certain procedures. "Employees are given incentive that says if you go here, you pay less," said Janet Faircloth, senior vice president of Aon’s health innovation team.
Reuters contributed to this report.